Autoclave Temperature and Pressure: How Saturated Steam Sterilization Works
Autoclave sterilization depends on three inseparable parameters: temperature, pressure, and time. Of these, the relationship between temperature and pressure is the most fundamental — and the least understood. In a steam autoclave, pressure does not merely support the process; it determines the temperature of the steam. Understanding this relationship explains why autoclaves achieve what boiling water cannot, and why air inside the chamber is the single greatest threat to a successful sterilization cycle.
The Three Main Parameters of Steam Sterilization
Every steam sterilization cycle is defined by three variables that must all be correct simultaneously:
| Parameter | Role |
|---|---|
| Temperature | The lethal agent — heat denatures microbial proteins and destroys cell structures |
| Pressure | Raises water's boiling point so steam exceeds 100°C; drives steam penetration into loads |
| Time | Ensures sufficient exposure for complete microbial kill across the entire load |
If any one of these three parameters is incorrect — or if air prevents steam from reaching the required temperature — sterilization fails.
Why Steam Kills Microorganisms
Microorganisms respond differently to heat depending on the temperature range:
- 0–7°C — Minimal or no multiplication; organisms survive
- 10–50°C — Ideal range for microbial multiplication and growth
- 62–100°C — Most vegetative bacteria die; spores survive
- Above 120°C (wet heat) — Bacterial spores are destroyed
This is why boiling water at 100°C is not sterilization — it cannot reliably kill spores. Steam under pressure raises the temperature above 100°C, which is the threshold needed to achieve true sterilization.
Steam kills through coagulation: the moist heat causes proteins inside microbial cells to denature and clump irreversibly, destroying enzymatic function and cell structure. This is fundamentally different from dry heat, which kills by oxidation — a slower, less efficient process requiring much higher temperatures and longer exposure times.
Why Water Content Makes Steam More Lethal Than Dry Heat
A key insight from microbiology is that microorganisms die more easily when they contain water. In a humid environment — such as inside a steam autoclave — microbial death occurs at lower temperatures and faster than in a dry environment. This is because moisture within the microbial cell amplifies heat transfer directly to the proteins and enzymes that sustain life.
Spores, which are the most resistant form of microbial life, still carry residual water. Saturated steam exploits this: the moisture condenses on and into the spore, allowing heat to penetrate and coagulate the proteins inside. Dry heat lacks this mechanism — it must reach far higher temperatures (typically 160–180°C for 1–2 hours) to achieve the same kill that steam achieves at 121–134°C in minutes.
Key Fact: Moist heat (steam) is far more effective than dry heat because microorganisms die faster when they contain water. In a humid environment, death occurs at lower temperatures and faster than in a dry environment — making saturated steam the most efficient sterilization agent available.
Microbial Death Rate and the Sterility Assurance Level
Microbial kill by heat is not instantaneous — it follows a predictable, logarithmic pattern. At 120°C, approximately 90% of microorganisms die per minute. This means that exposure time reduces the surviving population by one order of magnitude (one log₁₀) every minute. Starting from a heavily contaminated instrument with 1,000,000 (10⁶) organisms:
| Time at 120°C | Surviving Population |
|---|---|
| 0 minutes | 1,000,000 |
| 1 minute | 100,000 |
| 2 minutes | 10,000 |
| 12 minutes | 1 × 10⁻⁶ |
At 12 minutes, the probability of even one organism surviving falls below 1 in a million — this is the definition of sterility: a Sterility Assurance Level (SAL) of 10⁻⁶.
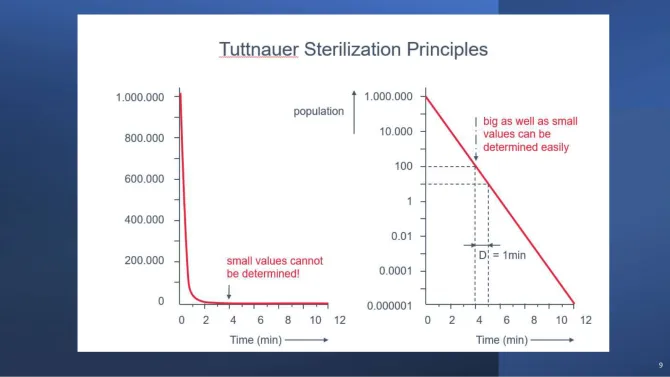
This logarithmic kill curve has an important practical consequence: sterility cannot be confirmed by simply checking that no bacteria are visible. At the endpoint, the population is so small it falls below any detectable threshold on a linear scale. This is why autoclave validation uses logarithmic biological indicators — specifically spore populations with known D-values — rather than direct bacterial counts.
D-Value and Z-Value
Two parameters quantify this logarithmic kill behaviour and form the scientific basis for designing and validating sterilization cycles:
D-value is the time required at a given temperature to reduce a specific microbial population by 90% (one log₁₀ reduction).
If a microbial population of 1,000,000 organisms has a D-value of 1.5 minutes at 121°C, one minute of exposure at that temperature reduces survivors to 100,000.
Z-value is the number of degrees of temperature change required to shift the D-value by a factor of 10 (one log₁₀). It is always expressed in °C.
For example, if the D-value at 121°C is 1.5 minutes and the Z-value is 10°C, then at 131°C the D-value drops to 0.15 minutes — the same kill is achieved ten times faster.
| Parameter | Definition | Unit |
|---|---|---|
| D-value | Time at temperature T to achieve 1 log₁₀ (90%) microbial reduction | minutes |
| Z-value | Temperature change needed to shift D-value by 1 log₁₀ | °C |
These two values are the critical inputs for calculating the Sterility Assurance Level (SAL) for any sterilization process. They become especially important when designing lethality-based or sub-lethal cycles — for example, terminal sterilization of parenteral products where precise lethality calculations are required by regulatory standards.
The left graph (linear scale) shows the population decline appearing to reach zero — but small values become invisible. The right graph (logarithmic scale) reveals the true kill profile and allows the precise point of SAL 10⁻⁶ to be measured and validated. This is the scientific foundation for using biological indicators (spore strips with known starting populations) to validate every autoclave cycle.
The Saturated Steam Pressure–Temperature Relationship
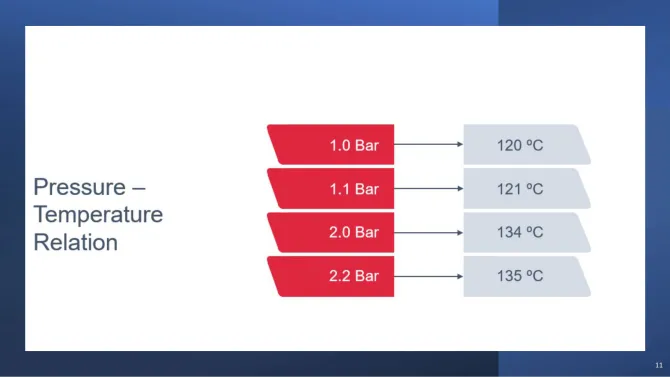
In a sealed autoclave chamber, steam pressure and temperature are not independent variables — they are governed by the properties of saturated steam. When water boils in a sealed vessel, every increase in pressure raises the temperature of the steam. The relationship is fixed and predictable:
| Pressure (bar gauge) | Temperature |
|---|---|
| 1.0 bar | 120°C |
| 1.1 bar | 121°C |
| 2.0 bar | 134°C |
| 2.2 bar | 135°C |
This is why autoclave gauges monitor both temperature and pressure simultaneously — they should always correspond to the values in this table. If the temperature reads lower than expected for a given pressure, air contamination in the chamber is almost certainly the cause.
Important: The pressure–temperature relationship above applies only to pure saturated steam. Any air mixed with the steam disrupts this relationship, causing temperature to read lower than pressure would predict. This is a diagnostic sign of incomplete air removal.
Minimum Holding Times at Sterilization Temperatures
Once the correct temperature is reached throughout the entire load, the autoclave must maintain it for a defined minimum period. These holding times are the scientifically established durations needed to achieve a sterility assurance level (SAL) of 10⁻⁶ — the elimination of all viable microorganisms with a probability of survival of less than 1 in a million.
| Temperature Range | Minimum Holding Time |
|---|---|
| 134–138°C | 3 minutes |
| 121–124°C | 15 minutes |
| 105–108°C | 2 hours |
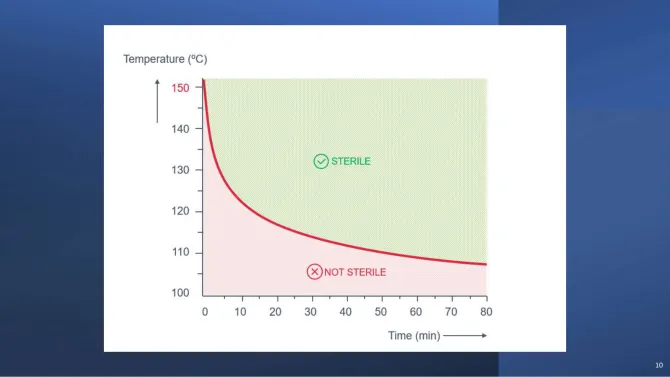
Higher temperatures allow shorter exposure times because the lethality of moist heat increases dramatically with temperature. A 3-minute cycle at 134°C delivers equivalent microbial kill to a 15-minute cycle at 121°C. This trade-off between temperature and time can be visualised as a lethality boundary: any combination of temperature and time that sits above the curve achieves sterility; anything below it does not.
This curve is why the holding time clock does not start until the entire load — not just the chamber air — reaches the target temperature. Dense or porous loads act as thermal mass and may lag behind the chamber by several minutes. For how these holding times translate into full cycle programs — including heat-up, drying, and total duration — see Autoclave Cycle Programs and Time Frames.
Key Fact: These are minimum holding times from the moment the entire load reaches the target temperature. Dense or complex loads may require additional time to fully equilibrate before the hold period begins.
Why Air Must Be Removed
Air is the primary enemy of steam sterilization. It causes two critical problems:
- It obstructs temperature rise. Air and steam are mixed gases. Where air is present, steam cannot reach its saturated state, so the temperature at that location will be significantly lower than the gauge pressure would predict.
- It prevents steam contact. Sterilization requires direct steam contact with all surfaces. Air pockets — particularly inside hollow instruments, fabric folds, or wrapped packages — create insulated zones where steam cannot penetrate.
The principle is simple: where there is air, there is no steam; where there is no steam, there is no sterilization.
Because air is denser than steam, it tends to settle to the bottom and low points of the chamber. This means that instruments on the lowest shelf of an improperly purged autoclave may not be sterilized even when the upper chamber shows correct temperature.
Two Air Removal Methods: Gravity vs. Pre-Vacuum
All autoclaves must remove air before steam can work. There are two fundamentally different approaches:
Gravity Displacement Autoclaves
In gravity (or downward displacement) autoclaves, steam enters from the top or back of the chamber. Steam is lighter than air, so it rises and pushes air downward. The air exits through a drain valve at the bottom of the chamber.
This process is passive and relies entirely on the density difference between air and steam. As a result:
- Air removal is slow and incomplete
- Approximately 5–10% of air may remain in the chamber after displacement
- Gravity autoclaves are less effective for porous loads, hollow instruments, or wrapped packages where air can be trapped internally
Gravity displacement is acceptable for simple loads: unwrapped solid instruments, liquids, and biohazardous waste. It is not suitable for complex or wrapped loads where air entrapment within the load itself is a concern.
Pre-Vacuum Autoclaves
Pre-vacuum autoclaves use a vacuum pump to actively remove air from the chamber before steam is introduced. The process typically runs multiple vacuum and steam-injection pulses (fractionated pre-vacuum) to progressively purge air from the chamber and from within the load.
After pre-vacuum conditioning:
- Less than 1% of air remains in the chamber
- Steam penetrates wrapped packs, porous materials, and hollow lumens far more effectively
- Sterilization cycles can run at 134°C with a 3-minute hold time instead of 15+ minutes
Pre-vacuum autoclaves are required for wrapped surgical instruments, textiles, porous loads, and hollow devices. They are the standard for hospital and surgical center sterilization. Because pre-vacuum autoclaves rely on the integrity of the vacuum system to guarantee air removal, daily verification using the Bowie-Dick test is mandated before the first production cycle.
A complete pre-vacuum sterilization cycle follows five distinct phases:
- Ejection of air by pre-vacuum — the vacuum pump actively removes air from the chamber and load before any steam is introduced
- Heating and pressure increase — steam is injected, raising chamber pressure and temperature to the target sterilization conditions
- Sterilization — the load is held at the target temperature for the minimum required time
- Exhaust — steam is vented, reducing chamber pressure to atmospheric
- Drying and cooling — residual moisture is removed, typically by post-vacuum; in laboratory systems, clean air through a HEPA filter is used to cool and dry the load without recontamination
| Feature | Gravity Autoclave | Pre-Vacuum Autoclave |
|---|---|---|
| Air removal method | Passive displacement by steam | Active vacuum pump |
| Residual air | ~5–10% | <1% |
| Typical cycle temperature | 121°C | 134°C |
| Minimum hold time | 15 minutes | 3 minutes |
| Suitable for wrapped loads | Limited | Yes |
| Suitable for hollow instruments | No | Yes |
| Suitable for porous loads | No | Yes |
These two principles map directly onto autoclave classification under EN 13060 — Class N for gravity displacement, Class B for full pre-vacuum. For a full breakdown of autoclave types, classes, and how to choose between them, see Types of Autoclave Sterilizers.
A Brief History: Why We Needed Autoclaves
Understanding the development of autoclaves puts the technology in perspective:
- 1670 — Van Leeuwenhoek discovers bacteria through microscopy, revealing the invisible microbial world
- 1862 — Pasteur proves bacteria multiply by division, that infection can be airborne, and that boiling kills bacteria
- 1870 — Bastian demonstrates that 100°C is insufficient to kill all microorganisms — some spores survive boiling
- 1880 — Chamberland manufactures the first autoclave designed to sterilize above 100°C using pressurized steam
The autoclave was invented specifically because boiling was not enough. Pressurized steam above 100°C was the solution that made reliable sterilization possible.
Standards and Regulatory References
Autoclave performance, cycle parameters, and validation requirements are governed by internationally recognized standards:
| Standard | Scope |
|---|---|
| AAMI ST79 | Comprehensive guide for steam sterilization in healthcare facilities |
| EN 285 | Large steam sterilizers for healthcare — performance requirements |
| EN 13060 | Small steam sterilizers — applies to dental and clinic-scale units |
| ISO 17665 | Moist heat sterilization of health care products |
| CDC Disinfection & Sterilization Guidelines | Evidence-based recommendations for sterilization practices |
Always consult your device's Instructions for Use (IFU) alongside these standards — manufacturer-validated parameters take precedence for specific equipment.
FAQ: Autoclave Temperature and Pressure
Why does an autoclave need pressure if steam already has heat?
Pressure raises water's boiling point above 100°C, allowing steam to reach 121–134°C. Without pressure, steam cannot exceed 100°C, which is insufficient to kill bacterial spores.
What is the relationship between pressure and temperature in an autoclave?
In a saturated steam environment, pressure and temperature are directly linked: 1.1 bar corresponds to 121°C, and 2.0 bar corresponds to 134°C. This relationship is fixed — any deviation indicates air contamination.
How long does an autoclave need to hold temperature?
Minimum holding times are 3 minutes at 134–138°C, 15 minutes at 121–124°C, and 2 hours at 105–108°C. Denser or more complex loads may require longer equilibration before the hold period begins.
Why is air so harmful to autoclave sterilization?
Air prevents steam from reaching saturation, lowers the actual temperature in air-contaminated zones, and blocks steam contact with surfaces. Areas with trapped air will not be sterilized even if the chamber gauge shows correct pressure and temperature.
What is the difference between a gravity and a pre-vacuum autoclave?
Gravity autoclaves displace air passively with steam, leaving 5–10% air residual. Pre-vacuum autoclaves actively pump air out, leaving less than 1% residual. Pre-vacuum is required for wrapped, hollow, and porous loads.
What temperature is needed to kill bacterial spores?
Bacterial spores require wet heat above 100°C. The standard parameters are 121°C for at least 15 minutes or 134°C for at least 3 minutes in a correctly purged steam autoclave.
Can I use boiling water instead of an autoclave?
No. Boiling water at 100°C kills most vegetative bacteria but cannot reliably kill bacterial spores. An autoclave's pressurized steam above 100°C is required for true sterilization (SAL 10⁻⁶).
What is a sterility assurance level (SAL) of 10⁻⁶?
SAL 10⁻⁶ means the probability of even one viable microorganism surviving on a sterilized item is less than 1 in 1,000,000. At 120°C, steam kills approximately 90% of organisms per minute — a logarithmic reduction that reaches SAL 10⁻⁶ after sustained exposure at the correct temperature.
Why does the holding time clock not start immediately when the cycle begins?
The holding time begins only once the entire load — including its core — has reached the target temperature. Dense loads, thick wrapping, and porous materials take time to equilibrate. The chamber pressure and temperature may be correct while the load interior is still warming up.
Conclusion
Steam sterilization works because of the precise, predictable relationship between pressure and temperature in saturated steam. Pressure elevates the steam temperature above 100°C — the threshold needed to destroy bacterial spores. Time ensures that lethal conditions persist long enough to eliminate all microbial life. And air removal, whether by gravity displacement or active pre-vacuum, is what allows steam to actually reach the load. When all three parameters are correctly controlled and air is eliminated, autoclaves achieve a sterility assurance level of 10⁻⁶ — the gold standard for medical, dental, and laboratory sterilization.